The R0 (R-naught or rate of infection) of psoriasis in the US adult population is currently at 3% or over 7.5 million people countrywide (Armstrong et al., JAMA Derm 2021). That’s not a negligible number by any account!
Background
Psoriasis is an ancient disease, with a fascinating history shrouded in mystery… to our days. Hippocrates termed the Greek Father of Medicine, who lived from 460-377 BCE, first described skin conditions by combining the words psora (itch) and lopoi (scaly, dry features), but at that time this may have included both psoriasis and leprosy.
What began as a skin disease is today considered in the medical literature a genetic and chronic autoimmune —or immune-mediated— disease consisting of the systemic inflammation of the body’s skin into collected or disperse patches of itchy and scaly skin, often visible as raised plaques or scales, all of it caused by the body’s immune system malfunction.
Gene Isolated
Until very recently, the origin and causes of psoriasis were cloaked in mystery, unknown. In 2005-2006 came a definitive breakthrough. The American Journal of Human Genetics published a peer-reviewed study where researchers isolated the PSORS1 gene for psoriasis susceptibility. That is the single biggest player in the gene pool identified to date, regulating how the immune system fought off the infection. The discovery of this common genetic variation helped explain why certain people were less prone than others to develop psoriasis (in the study, only 1 in 11 people with the PSOROS1 gene developed the disease) and opened an avenue of possibilities for psoriasis treatments with diminished side effects.
Effects
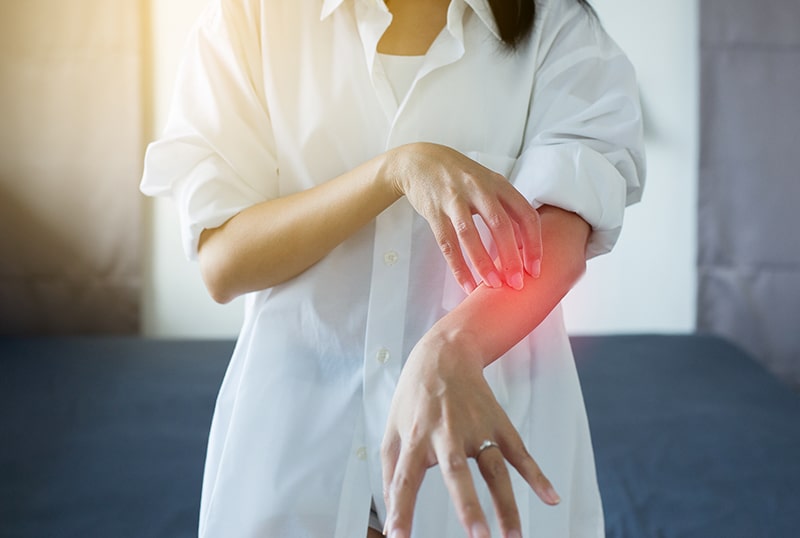
Psoriasis can manifest anywhere in the body, including eyelids, ears, lips, skin folds, hands, feet, and nails, although elbows, knees, and scalp are the most affected! Typically, normal skin cells grow and shed in a month. The malfunction means that an overactive immune system speeds up skin cell growth. And so, skin cells do this in roughly four days. Instead of shedding, they pile up on the skin surface, and the resulting plaques itch, burn, and sting.
Psoriasis is not infectious and affects women and men of all colors and ethnicities across the board. Its effects are visible beyond physical health, with general irritation, itchiness, and burning sensations at the forefront. It may also affect emotional health and stress handling and have a major impact on quality of life. Some people are deeply affected by what this condition does to their external appearance, even to the point of clothing selection, having to choose what you wear to keep the disease at bay.
In the worst cases, patients could develop psoriatic arthritis, with the ensuing tenderness, pain, and swelling of joints and connective tissue. As always, anyone’s best bet begins with a consultation with their GPs or healthcare provider.
Sources:
psoriasis.org/about-psoriasis/
papaa.org/learn-about-psoriasis-and-psoriatic-arthritis/common-questions/the-history-of-psoriasis/part-one-the-history-of-psoriasis/
webmd.com/skin-problems-and-treatments/psoriasis/news/20060317/gene-may-help-solve-psoriasis-mystery